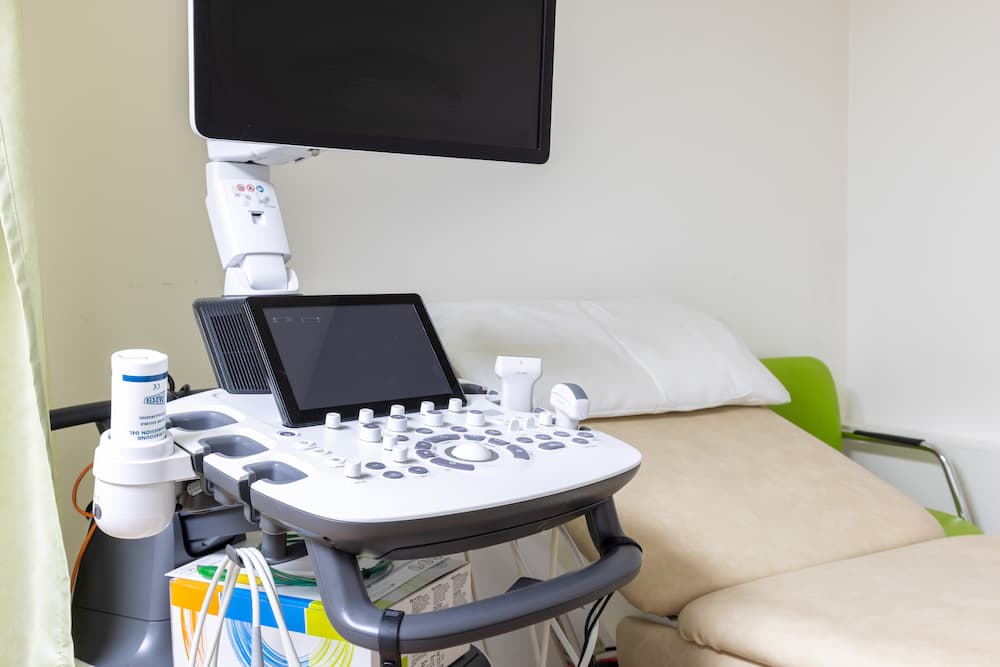
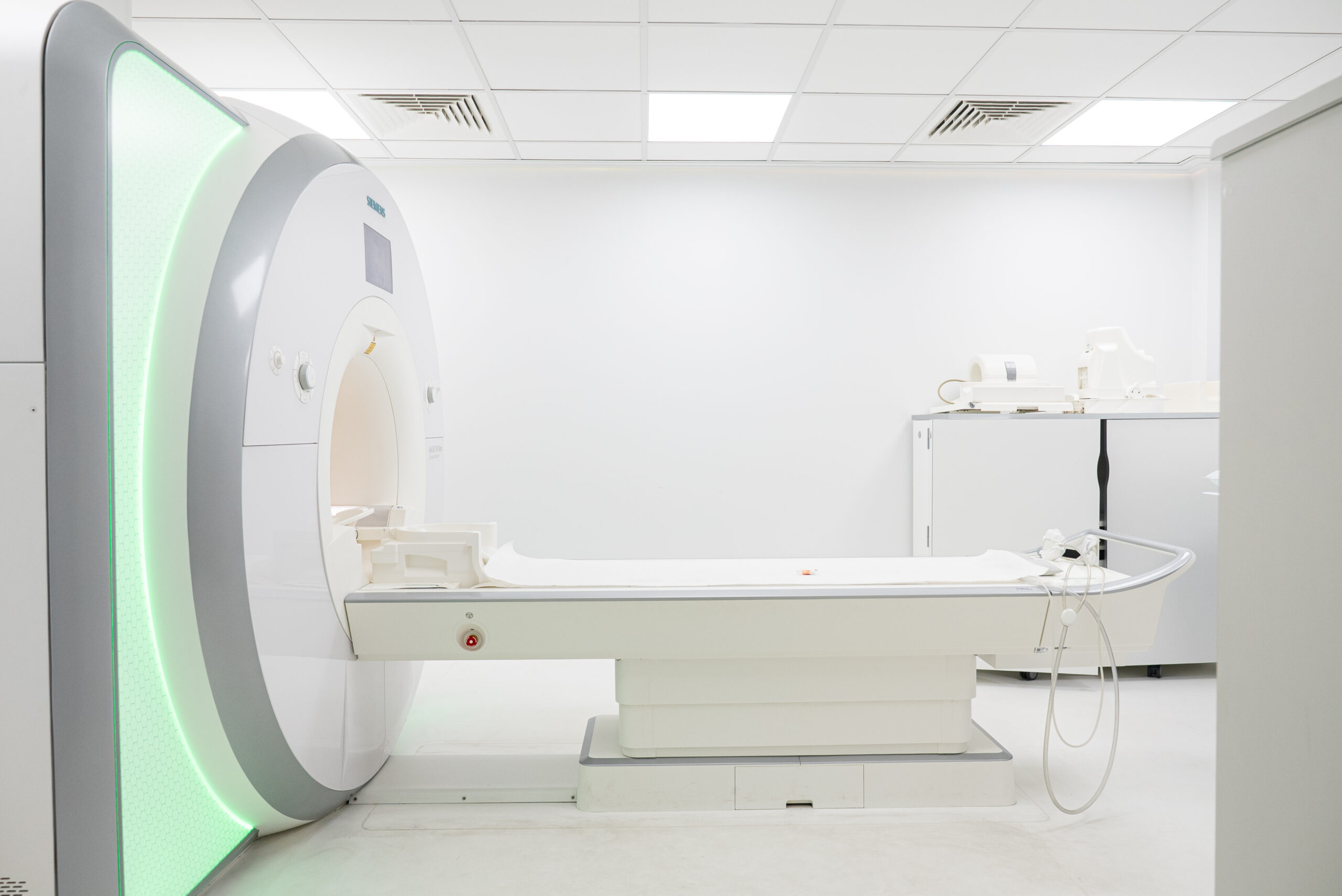
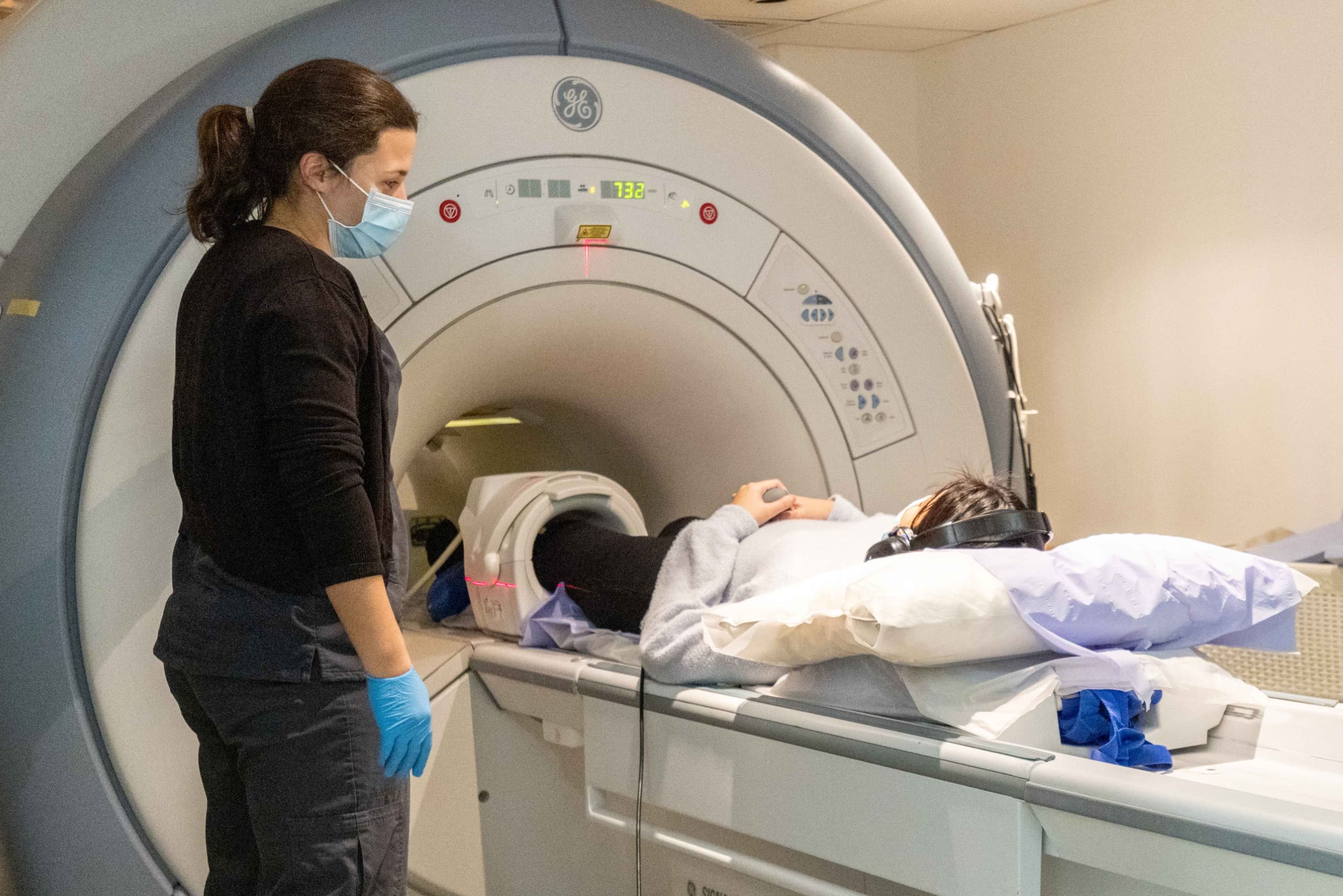
When it comes to musculoskeletal imaging, is MRI or ultrasound more effective?
The debate surrounding MRI vs Ultrasound ‘tos and fros’. When it comes to musculoskeletal imaging, both scan types can be used to assess most joints and conditions, but using the appropriate scan for the patient’s concern can make the diagnosis more accurate as well as saving the patient numerous investigations.
This blog will attempt to demystify some of the common misconceptions.
What are the differences between MRI and Ultrasound?
Firstly, most people feel that an MRI scan must somehow be superior to an Ultrasound scan because it is usually more expensive and the images obtained seem to be more elaborate. Referring clinicians can also look at MRI images and, importantly, show patients at the time of consultation. All of this makes MRI more tempting when it comes to MSK ailments.
However, it must be noted that Ultrasound has considerable advantages over MRI.
In general terms it is quicker and more easily accessible, especially as more and more sonographers and radiologists subspecialise in MSK Ultrasound. In the right hands Ultrasound can be an invaluable tool. Ultrasound does not have the claustrophobic issues that come with MRI. It is often cheaper, a factor that is an important consideration in the current financial climate faced by both the NHS and the private sector. Ultrasound also allows dynamic scanning with direct interaction between the operator and the patient, as well as allowing guided intervention to be performed at the same time. Here at Oryon Imaging all our ultrasound scans are performed by Consultant Radiologists.
When Should We Use MRI and When Should We Use Ultrasound (USS)?
If we take each MSK region in turn we can highlight conditions and situations when each one is more appropriate than the other.
Shoulder
If the clinical history is one of impingement and potential rotator cuff pathology then USS is preferred, USS can dynamically assess the rotator cuff and subacromial subdeltoid bursa and demonstrate active impingement. USS can then be used for an injection if clinically indicated or requested.
A shoulder MRI is perfect for assessing intra-articular pathologies such as labral abnormalities which would result in instability.
USS guided MR arthrograms can increase the sensitivity and specificity of labral pathologies.
Spine
USS has no role in the assessment of spinal conditions and MRI is the investigation of choice as it is vastly superior for imaging of the spine. A spinal MRI scan can exquisitely demonstrate disc pathology, vertebral anatomy and cord abnormalities.
Elbow and Wrist
If a tendinous pathology is suspected such as lateral epicondylitis (tennis elbow) or De Quervain’s Tenosynovitis – then go for USS. This will allow dynamic scanning with ability to add Doppler to demonstrate inflammation and also intervene with an injection if appropriate. However if a bony or ligamentous injury is suspected then MRI is far superior. So for scaphoid fractures and TFCC injuries MRI is the investigation of choice.
Hand
A combination of USS and MRI is used depending on local expertise to assess and look for tendon abnormalities such as pulley tears, or to look for synovitis.
Hip joint
If superficial hip structures need to be assessed such as the greater trochanter, gluteal tendons, iliopsoas or hamstrings then USS is very good for the same reasons as above. Dynamic scanning of the hip is particularly useful when assessing the snapping hip syndrome.
For internal hip issues, such as labral pathologies or CAM deformities and impingement then MRI or MR Arthrogram is preferred. MRI is usually also preferred for groin pathologies such as adductor sprains and sportsman’s hernia syndromes; although it must be said USS in the right hands can also give the diagnosis accurately and also guide intervention.
Knee
USS is very limited and only really useful for assessing the posterior fossa, the quadriceps and patella tendons.
A knee MRI scan is ideal for assessing all aspects of the knee and it is rare for a patient to have an USS of the knee. MRI can easily identify meniscal pathologies, ligamentous and tendinous injuries, as well as showing up characteristic bony oedema patterns associated with injuries.
Foot and Ankle
Also has specific indications for USS and others for MRI. If the clinical suspicion is of Achilles’ tendon or plantar fascia pathologies then USS is far superior to MRI, this is particularly the case if Achilles’ tendon rupture is suspected. In this case a dynamic scan is invaluable for the clinician to decide management. With both Achilles and plantar fascia diagnoses intervention must be done under USS to ensure safe distribution of the injectant – an incorrectly placed injection can lead to rupture and catastrophic results.
The flexor, extensor and peroneal tendons can be assessed using both MRI and USS and often with these complex patients they end up having both scans. MRI is gold standard for stress responses and stress fractures. MRI is also used to assess complex injuries such as the Lisfranc injury which can be unstable and require surgical intervention. Mortons neuromas can be assessed using both USS and MRI.
Lumps and bumps
It is widely accepted that USS should be the first line choice followed by MRI, if the diagnosis is either in doubt or sinister in nature.
To conclude
MRI and USS have their specific strengths and weaknesses. Understanding the uses of each modality appropriately can result in a much better, more accurate diagnosis with possible treatment and ultimately the right test for the right patient at the right time.
Dr Qaiser Malik, Consultant Radiologist
Oryon Imaging offers affordable private MRI scans, Ultrasound scans, X-rays and DEXA scans in the heart of Central London.